Mental Health and Wellbeing
Mental health promotion and mental illness prevention is integral to the work of York Region Public Health from service delivery right though to early identification and referral.
Mental Health Promotion in York Region
Mental health, or being mentally healthy, is the capacity of each and all of us to feel, think and act in ways that enhance our ability to enjoy life and deal with challenges or adversity. By building partnerships and engaging in multi-sectoral collaboration with community partners and health professionals, York Region Public Health demonstrates they are one of the many contributors to mental health promotion and can have a positive effect on the mental health and wellbeing of our community.
York Region Mental Health Resources and Referral Pathways
York Region Public Health's Perinatal Mental Health Pathway is a tool that enables health care providers to better connect their patients with community supports and resources. The pathway utilizes the Edinburgh Postnatal Depression Scale (EPDS) which is a validated tool recommended for the routine screening of individuals for perinatal depression and/or anxiety.
Early Years Support Services Registry is hosted by York Region Health Professionals and offers a comprehensive registry of community organizations throughout York Region for the birth to six year old population and their families.
Mental Health and the Social Determinants of Health
Income can have a significant impact on health. Not having enough money for basic necessities, such as healthy food and a warm place to stay, can negatively influence our opportunities for health including mental health.
Poverty: A Clinical tool for Primary Care Providers
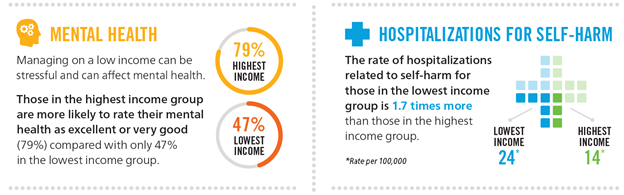
Income is a powerful social determinant of health. Addressing poverty is one of the most important roles faced by primary care providers. Research shows overwhelmingly that people who are unemployed, have low income, or find themselves in precarious employment have poorer health.1 Poverty increases the risk of cardiovascular disease, diabetes and depression as well as other chronic diseases.2 Individuals with mental illness or addiction often face poor mental health and experience stressful social and economic conditions such as low income and lack of access to housing.3 In York Region, those in the highest income group are more likely to rate their mental health as excellent or very good (79% in the highest income group compared to 47% in the lowest income group).4 In 2015, 197,030 (17.5%) of York Region residents were considered to have low income.5 While York Region is generally considered an affluent region, poverty still exists. 6
Poverty: A Clinical Tool for Primary Care Providers was developed by the Centre for Effective Practice in collaboration with the Ontario College of Family Physicians and Nurse Practitioners’ Association of Ontario to assist primary care providers address poverty with their clients. The tool offers specific resources for primary care providers and helps to start a conversation about poverty for those who are having difficulty making ends meet. The tool also assists primary care providers to screen for poverty and to provide support to their low income, vulnerable and marginalized patients.7
References
- Barnes, S., Block, S., Gardner, B, & Shaocott, M. (2013). Poverty is a Health Issue: Wellesley Institute Submission on the Ontario Poverty Reduction Strategy. Retrieved from https://www.wellesleyinstitute.com/wp-content/uploads/2013/09/Poverty-Reduction-Strategy-2013.pdf
- Centre for Effective Practice (2016). Poverty: A Clinical tool for Primary Care Providers (ON). Retrieved from https://cep.health/clinical-products/poverty-a-clinical-tool-for-primary-care-providers/
- Brien S, Grenier L, Kapral M.E., Kurdyak P, Vigod S. Taking Stock: A report on the quality of mental health and addictions services in Ontario [Government report online]. Toronto: Health Quality Ontario; 2015 [cited 2019 Mar19]. (ISBN 978-1-4606-7060-6 online). Available from: https://www.hqontario.ca/Portals/0/Documents/pr/theme-report-taking-stock-en.pdf
- Rapid Risk Factor Surveillance System (RRFSS) [2016]
- Regional Municipality of York, Community and Health Services Department, Strategies and Partnerships. Low income measures in Canada. Newmarket (ON): Regional Municipality of York; 2019
- Statistics Canada. Canada – Median household total income in 2015, by 2016 census division (CD) [Internet]. Ottawa, ON: Statistics Canada; [updated 2017 Aug 25; cited 2019 Mar 19]. Available from: https://www12.statcan.gc.ca/census-recensement/2016/rt-td/inc-rev-eng.cfm
- The College of Family Physicians of Canada (2016). Continuing Professional Development: Poverty: A Clinical Tool for Primary Care Providers. Retrieved from https://www.cfpc.ca/CFPC/media/Resources/Poverty/Poverty_flow-Tool-Final-2016v4-Ontario.pdf
Mental Health and Wellness in Pregnancy and Parenthood
Pregnancy or having a baby is not always easy. The adjustment to parenthood can be challenging for many families. Visit Mental Health and Wellness in Pregnancy and Parenthood for information on and referral to the Transition to Parenting program and other supports.
Healthy Aging and Mental Health
Healthy aging is an ongoing process of making the most of opportunities to maintain and improve physical, social and mental health. Social participation and social supports that allow us to maintain meaningful relationships with others are closely linked to good health and well-being throughout life. In older adults, social networks change and are influenced by illness, disability, and loss of friends and family members. Staying socially connected fosters meaningful opportunities to stay engaged in the community and with others and contributes to positive mental health.
Mental Health Resources for Older Adults
Mental Health for Seniors – York Region: Programs listed on centralhealthline.ca for older adults including preventive, diagnostic and treatment services in a variety of community and hospital-based settings to help achieve, maintain and enhance a state of emotional well-being, personal empowerment and the skills to cope with everyday demands.
Alzheimer Society - York Region: First Link® program connects families to local Alzheimer Society programs and other community services. First Link is about helping families make informed choices and to live better with dementia at every stage of the disease.
Best Practice Guidelines for Mental Health Promotion Programs: Older Adults 55+: A joint project of the Centre for Addiction and Mental Health, Dalla Lana School of Public Health, University of Toronto and Toronto Public Health
Support for Caregivers
Healthy Living Now: Powerful Tools for Caregivers is a free six week workshop for caregivers. Caring for a family member or friend with a chronic condition can be physically, emotionally, and financially draining. For more information and to register visit healthy-living-now.ca.
CHATS: Caregiver Support and Education services provide personal consultations and counselling and free support groups for caregivers.
Tobacco Use and Exposure Effects on Mental Health
Mental health improves with smoking cessation for the general population and those with mental health disorders.
Smoking cessation is associated with reduced depression, anxiety, and stress and improved positive mood and quality of life when compared to continuing to smoke for the general population and those with mental health disorders. Help to dispel the myth that smoking tobacco has mental health benefits. For more information on available cessation services visit york.ca/tobacco
Mental health risks of tobacco smoking
- People who smoke have a 45% higher risk of developing dementia including Alzheimer’s disease than those who don’t smoke.
- Early onset of tobacco use, current and past tobacco use are associated with increased risk of suicidal thoughts and attempts.
- Current smoking is associated with a nearly two-fold increased risk of depression relative to those who never smoked and those who quit smoking.
Mental health improves with smoking cessation
- Smoking cessation is associated with reduced depression, anxiety, and stress and improved positive mood and quality of life compared with continuing to smoke both in the general population and in those with mental health disorders.
- Smoking cessation is associated with a decreased risk of suicide attempts.
Patients may benefit from screening for tobacco use as part of a mental health assessment. A three-step brief intervention by health care practitioners can increase the likelihood of quitting.
- Ask all patients about current/past tobacco use
- Advise how smoking and quitting affects health and
- Refer as needed to a cessation program.
Let your patients know that by quitting smoking they can improve their mental health. For more information on available cessation services, visit york.ca/tobacco
Mental Health and Substance Use
The relationship between mental health and substance use is complex. They might develop independently as a result of common risk factors or one might lead to the other. Young people aged 15 to 24 are more likely to experience mental illness and/or substance use disorders than any other age group.2 Prevention and early intervention is key. Concurrent disorders require specialized services. Care for individuals with concurrent disorders is typically fragmented and not well integrated to meet client needs for both conditions.1 When providing care, it is important to provide well-integrated care by considering both co-occurring conditions, ensuring client-centered care, and increased client participation. Consider the resources in the references section below.
External Links and Resources
Registered Nurses Association of Ontario: RNAO Best Practice Guidelines on Engaging Clients Who Use Substances
Public Health Ontario’s Interactive Opioid Tool
The Interactive Opioid Tool allows users to explore the most recent opioid-related morbidity and mortality data including emergency department visits, hospitalizations and deaths. Results can be viewed by public health unit, local health integration network, age, sex, and in some cases, drug type.
Ontario Prescription Opioid Tool
The Ontario Prescription Opioid Tool allows public access to data related to indicators for opioid prescribing in the province from 2012 onwards using data housed at ICES. This tool was created by the Ontario Drug Policy Research Network (ODPRN) in collaboration with ICES, Public Health Ontario and integrating other stakeholder input, including the Ministry of Health and Long-Term Care, Public Health Units (PHUs), and Local Health Integration Networks (LHINs). It was made to complement Public Health Ontario’s interactive tool on opioid-related harms and will be updated on an approximately quarterly basis.
Connex Ontario
ConnexOntario provides free and confidential health services information for people experiencing problems with alcohol and drugs, mental illness and/or gambling. System navigation and information service is live-answer 24/7, confidential, and free. Contact 1-866-531-2600
College of Family Physicians of Canada: Helping Patients Reduce Alcohol-related Risks and Harms
Collaboration for Addiction and Mental Health Care: Best Advice
Ontario Centre of Excellence for Child and Youth Mental Health: Pathways to Care for Youth with Concurrent Mental Health and Substance Use Disorders
Centre for Addiction and Mental Health: Concurrent Substance Use and Mental Health Disorders An Information Guide
Canadian Centre on Substance Abuse and Addiction: When Mental Health and Substance Abuse Problems Collide
References
- Canadian Centre on Substance Use and Addiction (2013). When mental health and substance abuse problems collide. Retrieved from https://www.ccsa.ca/when-mental-health-and-substance-abuse-problems-collide-topic-summary
- The Centre for Addiction and Mental Health (2019). CAMH Mental Illness and Addiction: Facts and Statistics. Retrieved from https://www.camh.ca/en/driving-change/the-crisis-is-real/mental-health-statistics
Mental Health and Sexual Health
When an individual has good mental health, they are equipped to make better decisions about their sexual health. Many individuals struggle with the challenges that can arise around their sexuality and mental health, due to a lack of information, level of comfort and anticipated lack of support accompanied with a fear of judgement and being stigmatized. It is imperative for physicians and other health care professionals to ask questions about an individual’s sexuality and their mental health in a respectful, open and sensitive manner as part of their overall health care.
Below is a list of resources that are very helpful when taking an individual’s mental health into consideration while addressing their sexual health concerns.
- york.ca/sexualhealth – Information regarding what the sexual health clinics program offers to the public including information about the services offered through sexual health clinics
- Mind Your Business – a handbook for health care providers - When it comes to mental health and sexual health, individuals may feel hesitant to access health care due to concerns around or previous experiences of stigma and discrimination. This handbook includes scenarios, discussion prompts, and tips for health care professionals
- Gender Affirming Clinic CMHA York and South Simcoe offers medical and counselling services for trans and gender diverse individuals at two separate locations (Aurora and Vaughan) twice a month @email
- Rainbow Resources of York Region provides safe, inclusive social and recreational spaces for the 2SLGBTQ+ community.
- Pflag Canada - York Region – support meeting for family members of LGBTQ+ individuals
- MOBYSS (Mobile York South Simcoe) offers a safe space to talk to a medical or mental health professional in a warm, welcoming, friendly environment. They offer sexual health services among other services.
- Here to Help – Sex, Intimacy and Mental Well-Being - reviews the importance of positive mental well-being and how a struggle with mental illness can affect one’s sexual desires and interests.
External Links
Canadian Mental Health Association: CMHA branches across Canada provide a wide range of innovative services and supports to people who are experiencing mental illness and their families. These services are tailored to the needs and resources of the communities where they are based. One of the core goals of these services is to help people with mental illness develop the personal tools to lead meaningful and productive lives.
Canadian Mental Health Association – Bounce Back Program: Reclaim Your Health: Bounce Back is an evidenced-based program designed to help adults overcome symptoms of mild to moderate depression, low mood, or stress with or without anxiety.
Centre for Addictions and Mental Health: The Centre for Addiction and Mental Health (CAMH) is Canada's largest mental health and addiction teaching hospital, as well as one of the world's leading research centres in the area of addiction and mental health. CAMH combines clinical care, research, education, policy development and health promotion to help transform the lives of people affected by mental health and addiction issues.
ConnexOntario – Addiction, Mental Health and problem Gambling: Helpline: ConnexOntario provides free and confidential health services information for people experiencing problems with alcohol and drugs, mental illness and/or gambling. Funded by the Government of Ontario. Information and referral service is live-answer 24/7, confidential, and free.
Kids Help Phone: Kids Help Phone is a Canadian and world leader known for their expertise and continuous innovation as Canada’s only 24/7 counselling and information service for young people. Since 1989, their trained, professional counsellors have been listening to kids, often when no one else can or will.
Children's Mental Health Ontario : Children's Mental Health Ontario (CMHO) is the association representing Ontario’s publicly-funded Child and Youth Mental Health Centres. CMHO works to identify and develop solutions to important policy issues affecting the child and youth mental health sector. Their primary goal is to promote a coordinated and high quality system of care that puts children, youth and families first.
Community Mental Health and Addictions Crisis Response Service: A 24/7 service for people living in York Region, South Simcoe, or North York who are having a mental health crisis, and their family or friends
1-855-310-COPE (2673)
TTY number: 1-866-323-7785
Promoting Mental Health – Common Language: How do YOU talk about mental health promotion?
There is growing discussion about mental health in Ontario and the way we talk about it matters. This video, created by the CAMH Health Promotion Resource Centre, explains the separate but interconnected concepts of mental health and mental illness, and what it means to ‘promote mental health’ in ourselves and in our communities.